Overview of Wound Care Assessment
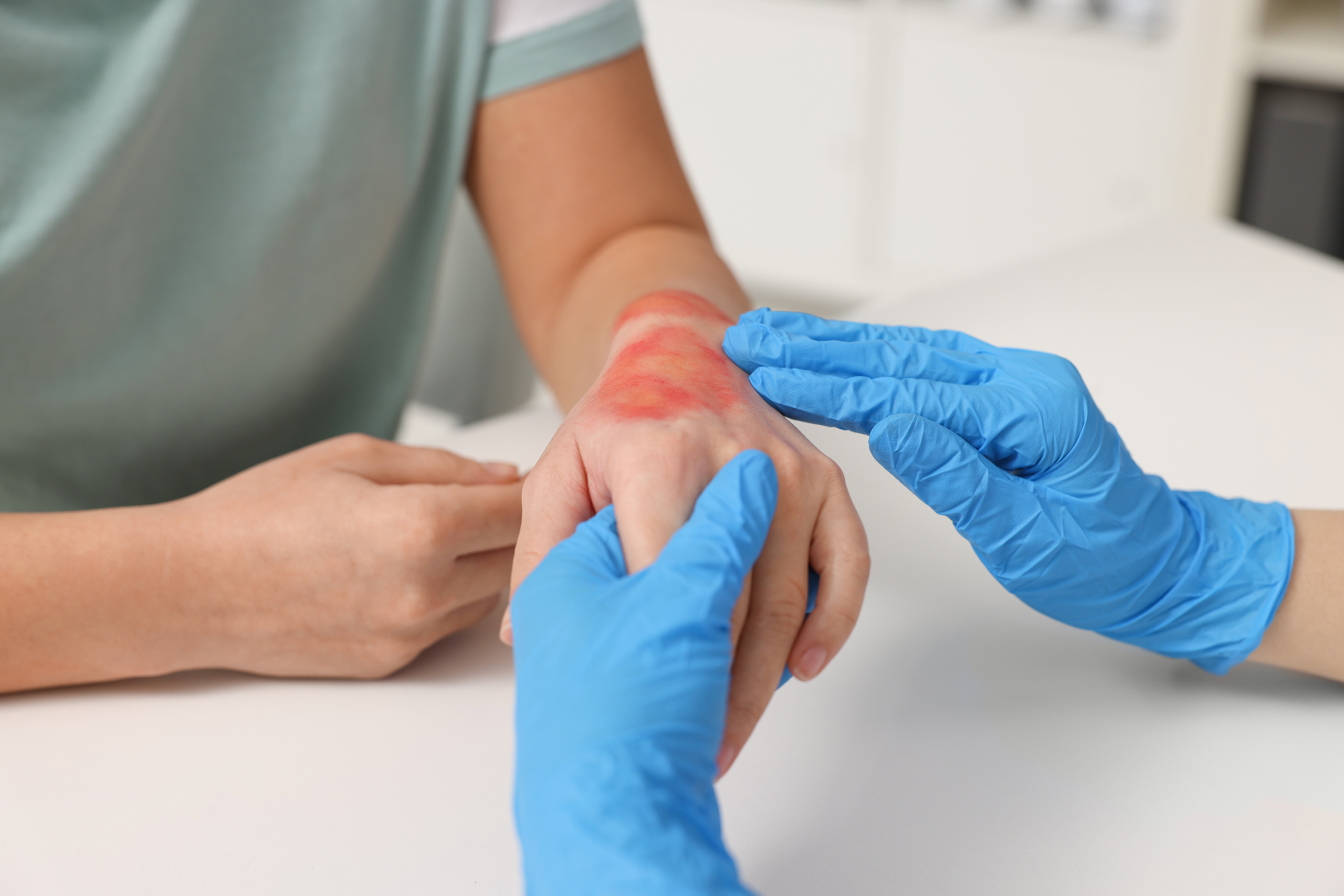
Wound care assessment is a structured clinical process used to evaluate the condition of a wound and determine the most appropriate treatment approach. It plays a critical role in identifying how a wound is progressing and whether healing is occurring as expected. Healthcare professionals rely on wound care assessment to make informed decisions about dressing selection, infection control, and intervention strategies. The process involves both visual and tactile evaluation combined with patient history and symptom reporting. A thorough assessment helps prevent complications that may delay healing or worsen the condition. It also supports continuity of care across different healthcare providers. Accurate evaluation ensures that treatment plans remain aligned with the patient’s evolving needs.
Wound care assessment is not a one-time activity but a continuous process that adapts to changes in the wound environment. Clinicians must consistently monitor key indicators such as tissue type, moisture balance, and signs of infection. Proper assessment supports early detection of complications, which is essential for effective wound management. It also provides baseline data that can be used for comparison over time. Documentation of findings is equally important in maintaining accurate clinical records. Without structured assessment, treatment outcomes may become unpredictable. This makes wound care assessment a foundational skill in healthcare practice.
Importance of Accurate Wound Evaluation in Clinical Practice
Accurate wound care assessment is essential for ensuring optimal patient recovery and preventing complications. When wounds are properly evaluated, clinicians can tailor interventions to the specific needs of the patient. This reduces the risk of infection, tissue deterioration, and prolonged healing time. In clinical settings, precise assessment contributes to better resource allocation and treatment efficiency. It also minimizes unnecessary interventions that may burden the patient. Consistency in evaluation improves communication among healthcare teams. This ultimately leads to improved patient outcomes and satisfaction.
Healthcare systems also benefit financially from accurate wound evaluation. Proper assessment reduces hospital readmissions and long-term treatment costs. It ensures that patients receive appropriate care at the right time. Clinical decision-making becomes more reliable when based on objective data. It also supports evidence-based practice in wound management. Patients experience better quality of life when wounds heal efficiently. Overall, wound care assessment is a critical component of effective healthcare delivery.
Anatomy of Skin and Wound Healing Phases
Understanding skin anatomy is essential for effective wound care assessment. The skin consists of multiple layers that serve protective and regulatory functions. These include the epidermis, dermis, and subcutaneous tissue. Each layer plays a role in the healing process after injury. Damage to these layers triggers a complex biological response. This response is essential for tissue repair and regeneration.
Wound healing occurs in several overlapping phases. The hemostasis phase involves clot formation to stop bleeding. The inflammatory phase focuses on cleaning the wound through immune response. The proliferative phase supports tissue growth and wound closure. The maturation phase strengthens newly formed tissue over time. Each phase must progress properly for complete healing to occur. Disruptions in any phase can delay recovery and complicate treatment.
Types of Wounds and Their Clinical Characteristics
Wounds are classified based on their cause, duration, and depth. Acute wounds typically result from surgery or trauma and follow a predictable healing pattern. Chronic wounds, however, fail to progress through normal healing stages. Examples include diabetic ulcers, pressure injuries, and venous ulcers. These wounds require specialized wound care assessment due to their complexity. Proper classification helps guide treatment strategies.
Partial-thickness wounds affect the epidermis and part of the dermis. Full-thickness wounds extend deeper into underlying tissues. Infection status also influences wound classification. Clean wounds have minimal contamination, while contaminated wounds show bacterial presence. Infected wounds display visible signs of microbial activity and inflammation. Understanding these distinctions is essential for effective clinical decision-making. Each wound type requires a tailored assessment approach.
Initial Patient Evaluation and Health History Review
A comprehensive wound care assessment begins with a detailed patient history. Clinicians evaluate underlying medical conditions that may affect healing. Conditions such as diabetes, vascular disease, and immune disorders are particularly relevant. Medication use is also reviewed to identify drugs that may impair recovery. Lifestyle factors such as smoking and nutrition significantly influence wound healing outcomes. Mobility limitations are also considered during evaluation.
A structured approach to patient evaluation often includes:
- Reviewing chronic illnesses and comorbidities
- Assessing current medications and possible side effects
- Evaluating nutritional status and hydration levels
- Identifying lifestyle habits affecting healing
- Examining previous wound history and healing patterns
This information provides context for interpreting wound characteristics. It also helps identify risk factors that may delay recovery. A complete health history supports more accurate wound care assessment. It ensures that treatment plans address both local and systemic influences.
Systematic Wound Assessment Process
A structured wound care assessment involves careful examination of multiple wound characteristics. Clinicians begin by identifying the wound location and anatomical context. Measurements of length, width, and depth are taken using standardized methods. The condition of wound edges is evaluated for signs of undermining or maceration. Surrounding skin is also assessed for redness, swelling, or discoloration. Tissue composition is classified based on appearance and viability.
Exudate levels are carefully documented, including color, consistency, and volume. Odor is assessed as it may indicate infection or tissue breakdown. Pain levels are recorded based on patient feedback and clinical observation. Each element contributes to a complete understanding of wound status. Consistency in assessment ensures reliable tracking of healing progress. This structured process supports accurate clinical decision-making.
Wound Measurement Techniques and Documentation Standards
Accurate measurement is a key component of wound care assessment. Clinicians use rulers, probes, and digital tools to obtain precise dimensions. Measurements must be consistent to ensure reliable comparisons over time. Photographic documentation is often used to support visual tracking. Digital systems improve accuracy and reduce human error. Standardized documentation ensures uniformity across healthcare teams.
Clear documentation should always include objective data. Descriptions must avoid subjective language and focus on measurable findings. Proper record-keeping supports legal compliance and clinical accountability. It also enhances communication between different care providers. Consistent documentation improves continuity of care. This ensures that all healthcare professionals are aligned in treatment planning.
Tools and Technologies Used in Wound Care Assessment
Modern wound care assessment benefits from advanced technologies. Digital imaging systems allow for precise wound visualization. Measurement software improves accuracy in tracking wound size changes. Mobile applications enable real-time documentation and monitoring. Electronic health records integrate assessment data for better coordination. Ultrasound tools can assess deeper tissue involvement.
These technologies enhance clinical efficiency and reduce errors. They also support remote monitoring in some healthcare settings. Automation helps standardize wound evaluation processes. Data-driven insights improve treatment planning. Technology continues to transform how wound care assessment is performed in clinical environments.
Infection Identification and Risk Indicators
Infection is a major concern in wound care assessment. Early detection is essential for preventing complications. Local signs include redness, warmth, swelling, and increased pain. Systemic signs may involve fever and elevated white blood cell count. Biofilm formation can complicate treatment and delay healing. Identifying infection early improves clinical outcomes.
Healthcare providers must remain vigilant for subtle changes in wound appearance. Changes in exudate or odor may indicate infection onset. Risk factors such as diabetes increase susceptibility. Proper assessment helps guide timely intervention. Infection control is a critical part of wound management. Early treatment significantly improves healing potential.
Pain Assessment in Wound Management
Pain evaluation is an important component of wound care assessment. Patients may experience varying levels of discomfort depending on wound type. Pain scales help quantify subjective experiences. Clinicians assess pain during rest and movement. Dressing changes may also trigger discomfort. Understanding pain patterns helps guide treatment decisions.
Pain can indicate underlying complications such as infection or tissue damage. Effective pain management improves patient compliance. It also enhances overall quality of care. Communication between patient and clinician is essential. Regular pain assessment ensures timely adjustments to treatment plans.
Wound Bed Preparation Principles
Wound bed preparation is essential for successful healing. It involves removing non-viable tissue and controlling bacterial load. Moisture balance must be carefully maintained. Healthy tissue growth is encouraged through proper wound environment management. Debridement may be required in certain cases. This process supports faster healing.
Effective wound care assessment guides wound bed preparation decisions. Clinicians evaluate tissue quality before intervention. Maintaining a clean wound environment is critical. Proper preparation reduces complications and improves outcomes. It is a foundational principle in wound management.
Dressing Selection Based on Wound Assessment Findings
Dressing selection is directly influenced by wound care assessment results. Different wounds require different moisture and protection levels. Foam dressings are suitable for high exudate wounds. Hydrocolloid dressings support moist healing environments. Alginate dressings are effective for heavily draining wounds. Hydrogel dressings support dry wounds.
Choosing the correct dressing improves healing efficiency. It also reduces patient discomfort and infection risk. Regular reassessment ensures appropriate dressing adjustments. Clinicians must evaluate wound changes consistently. Dressing selection is a dynamic process guided by assessment findings.
Chronic Wounds vs Acute Wounds Assessment Differences
Chronic wounds require more detailed wound care assessment due to their complexity. They often fail to progress through normal healing stages. Acute wounds typically follow predictable healing timelines. Chronic wounds may require long-term management strategies. Tissue response differs significantly between the two types. Chronic wounds often show delayed healing signs.
Assessment priorities vary depending on wound classification. Chronic wounds require frequent monitoring and intervention. Acute wounds focus on ensuring proper initial healing. Understanding these differences improves treatment planning. Each wound type demands a tailored clinical approach.
Special Populations Considerations
Certain populations require modified wound care assessment approaches. Diabetic patients face increased risk of delayed healing. Elderly individuals often have fragile skin and reduced regeneration capacity. Immunocompromised patients are more susceptible to infection. Pediatric patients require gentle and specialized care techniques. Each group presents unique clinical challenges.
Assessment must consider underlying physiological differences. Tailored strategies improve healing outcomes. Clinicians must adapt evaluation techniques accordingly. Patient safety remains a top priority. Special populations require careful monitoring throughout treatment.
Interdisciplinary Role in Wound Care Assessment
Wound management involves collaboration among healthcare professionals. Nurses often perform routine wound care assessment. Physicians oversee treatment planning and medical intervention. Nutritionists support healing through dietary planning. Physical therapists assist with mobility improvement. Each role contributes to patient recovery.
Team-based care enhances treatment effectiveness. Communication among professionals ensures coordinated management. Interdisciplinary collaboration improves outcomes. It also reduces treatment delays. Wound care benefits greatly from shared expertise.
Common Documentation Errors and How to Avoid Them
Documentation errors can compromise wound care assessment accuracy. Inconsistent measurements are a common issue. Missing updates affect treatment continuity. Subjective descriptions reduce clarity. Standardized terminology helps avoid confusion. Proper training reduces documentation mistakes.
Accurate records support effective clinical decision-making. They also ensure legal compliance. Consistency is essential in healthcare documentation. Regular audits improve documentation quality. Clear records enhance patient care coordination.
Evidence-Based Guidelines in Wound Assessment
Evidence-based practice is central to modern wound care assessment. Clinical guidelines provide standardized evaluation methods. Research supports effective treatment strategies. Validated tools improve assessment accuracy. Continuous education ensures updated clinical knowledge. Evidence-based care improves patient outcomes.
Healthcare professionals must stay informed about new research. Guidelines evolve based on emerging evidence. Applying best practices enhances treatment success. Standardization reduces variability in care. Evidence-based assessment is essential in modern healthcare.
Patient Education and Self-Monitoring Practices
Patient involvement is important in wound care assessment. Education helps patients understand their condition. Proper hygiene practices reduce infection risk. Patients must recognize warning signs of complications. Self-monitoring improves early detection of changes. Compliance with treatment plans supports healing.
Educated patients contribute to better outcomes. They are more likely to follow care instructions. Communication with healthcare providers is essential. Empowering patients improves long-term recovery. Education is a key component of wound management.
When to Escalate Care or Refer to Specialists
Certain wound conditions require specialist intervention. Non-healing wounds may indicate underlying complications. Signs of deep infection require urgent attention. Surgical evaluation may be necessary in severe cases. Referral ensures access to advanced treatment options. Timely escalation improves patient outcomes.
Clinicians must recognize when standard care is insufficient. Early referral prevents further complications. Specialist involvement enhances treatment effectiveness. Clear referral pathways improve healthcare efficiency. Escalation is a critical part of wound management.
Frequently Asked Questions
What is included in wound care assessment?
Wound care assessment includes evaluation of wound size, depth, tissue type, exudate, odor, pain, and surrounding skin condition.
How often should a wound be assessed?
Frequency depends on wound severity, but most wounds require regular monitoring ranging from daily to weekly evaluations.
What are key indicators of healing progress?
Reduction in wound size, healthy granulation tissue formation, and decreased exudate are common indicators.
How do chronic wounds differ from acute wounds in assessment?
Chronic wounds require ongoing monitoring and show delayed healing compared to acute wounds.
What tools are commonly used in assessment?
Tools include rulers, digital imaging systems, probes, and electronic health record systems.
When should a specialist be consulted?
Specialists should be consulted when wounds fail to heal, show signs of infection, or require advanced treatment.
Takeaway
Wound care assessment serves as the foundation of effective wound management by guiding clinical decisions, improving healing outcomes, and preventing complications through structured and evidence-based evaluation practices.