Understanding Sever Wound Surgery
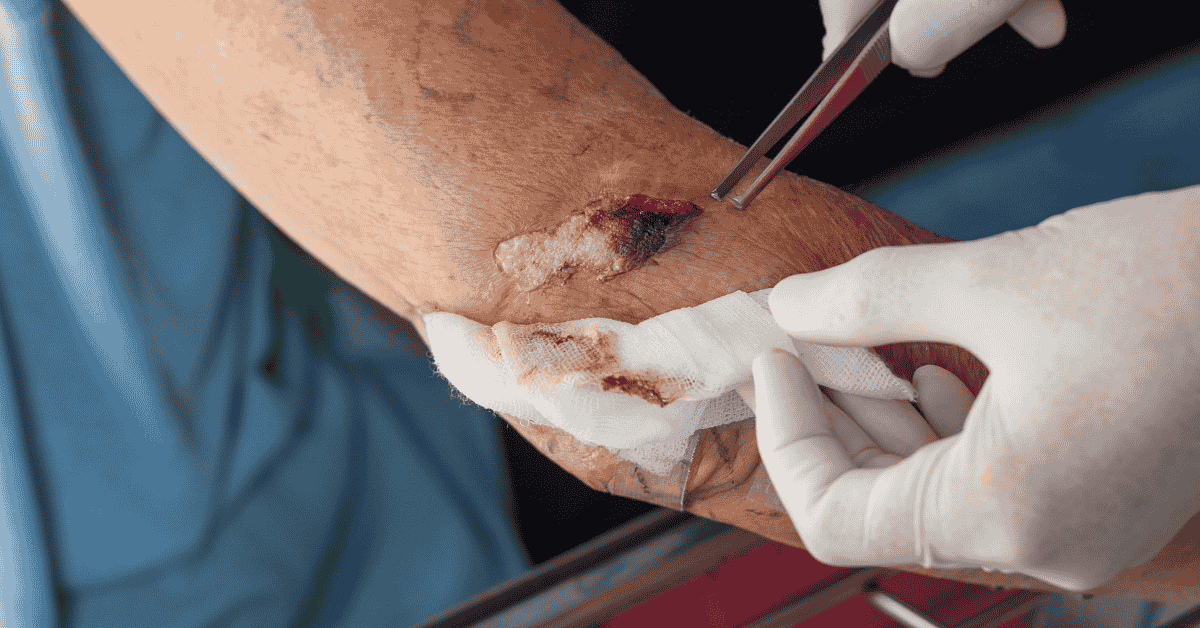
Sever wound surgery refers to a specialized medical intervention designed to treat deep, complex, and often life-threatening injuries that involve significant damage to skin, muscle, tendons, blood vessels, or bone. This type of surgical care is typically required when a wound cannot heal properly through basic medical treatment or stitching alone. In many situations, sever wound surgery is performed in emergency settings where immediate action is necessary to prevent infection, blood loss, or permanent tissue damage. The procedure is a critical component of trauma medicine and plays an essential role in saving both limbs and lives. Medical teams often evaluate the extent of damage carefully before deciding the best surgical approach. Sever wound surgery is not limited to one technique, as it may involve multiple reconstructive and corrective procedures depending on injury severity. It is widely used in hospitals with trauma units and specialized surgical departments.
Primary Causes Leading to Severe Wounds
Severe wounds that require sever wound surgery often result from high-impact physical trauma such as car accidents, motorcycle crashes, or industrial workplace incidents. These injuries can also occur during falls from significant heights, especially in construction environments where safety measures may be insufficient. Sports injuries involving high force impact or collisions can also lead to deep tissue damage requiring surgical repair. Animal bites, particularly from large animals or infected sources, may introduce both structural damage and bacterial contamination. Burns caused by fire, chemicals, or electricity can destroy multiple layers of skin and underlying tissue, making surgical intervention necessary. Penetrating injuries from sharp objects, including glass or metal, may sever blood vessels or nerves, increasing the complexity of treatment. Chronic health conditions like diabetes or vascular disease can worsen minor wounds, turning them into severe surgical cases due to poor healing capacity.
Medical Evaluation Before Sever Wound Surgery
Before performing sever wound surgery, medical professionals conduct a detailed evaluation to understand the extent of the injury. This includes checking vital signs such as heart rate, blood pressure, and oxygen levels to ensure the patient is stable enough for surgery. Imaging tests like X-rays, CT scans, and MRI scans help doctors assess damage to bones, muscles, and internal structures. Blood tests are often performed to detect infection, blood loss, or clotting issues that could affect surgical outcomes. The wound is carefully examined to determine contamination levels and the presence of foreign materials. Physicians also assess how urgently surgery is needed based on tissue viability and risk of complications. This evaluation process ensures that the surgical plan is safe, precise, and tailored to the patient’s condition.
Indications for Sever Wound Surgery
Sever wound surgery becomes necessary when there is extensive tissue destruction that cannot heal naturally or with basic medical care. One major indication is the presence of necrotic or dead tissue that must be removed to prevent infection from spreading. Severe bleeding that cannot be controlled through external pressure is another urgent reason for surgical intervention. Deep wounds exposing muscles, tendons, or bones require surgical closure and reconstruction. Infections that penetrate deep into tissue layers also demand surgical cleaning and treatment. Open fractures where bones are exposed or shattered often require surgical stabilization. Sever wound surgery is also indicated when blood flow to a limb is compromised, risking tissue death without intervention.
Types of Sever Wound Surgery Procedures
There are several types of procedures involved in sever wound surgery, each tailored to specific injury conditions. Surgical debridement is one of the most common techniques, involving the removal of damaged or infected tissue to promote healing. Wound closure techniques, including suturing and stapling, are used when tissue can be safely reconnected. Skin grafting is another method where healthy skin is transferred from one part of the body to cover the injured area. Flap surgery involves moving tissue along with its blood supply to reconstruct complex wounds. Microvascular surgery is used to repair damaged blood vessels and restore proper circulation. In cases involving bone damage, orthopedic surgical techniques may be required to stabilize and realign skeletal structures.
Surgical Planning and Preparation
Proper planning is essential before performing sever wound surgery to ensure safety and effectiveness. The medical team first stabilizes the patient to prevent further deterioration of their condition. Anesthesia is selected based on the severity and location of the wound, ranging from local to general anesthesia. The surgical site is thoroughly cleaned to reduce the risk of infection during the procedure. Doctors also prepare antibiotics to be administered before, during, and after surgery. Imaging results are reviewed carefully to guide surgical precision and avoid complications. The surgical team coordinates responsibilities to ensure smooth execution of each step during the operation.
Step-by-Step Surgical Process in Sever Wound Surgery
The surgical process begins with a detailed exploration of the wound to assess internal damage. Damaged or dead tissue is carefully removed through debridement to create a clean healing environment. Bleeding is controlled using surgical tools such as cauterization devices or ligation techniques. Surgeons then repair damaged muscles, tendons, or blood vessels depending on the injury. If necessary, grafts or flaps are applied to replace missing tissue and restore coverage. The wound is then closed using appropriate techniques to minimize tension and promote healing. Drainage systems may be installed to prevent fluid buildup and reduce infection risk.
Post-Surgical Wound Care and Monitoring
After sever wound surgery, proper wound care is essential for successful recovery. Dressings are changed regularly under sterile conditions to prevent infection. Patients are closely monitored for signs of complications such as swelling, redness, or unusual discharge. Pain management is provided through medications tailored to patient needs. Antibiotics are continued to ensure that infection does not develop after surgery. Follow-up visits allow doctors to evaluate healing progress and adjust treatment plans if necessary. Early physical movement may be encouraged depending on the injury location to prevent stiffness and improve circulation.
Healing Phases After Sever Wound Surgery
The healing process following sever wound surgery occurs in several stages that support tissue recovery. The first stage involves clot formation to stop bleeding and protect the wound. The inflammatory stage follows, where the body works to remove bacteria and damaged cells. During the proliferative stage, new tissue begins to form, gradually closing the wound. The final remodeling stage strengthens the repaired tissue and improves flexibility. Factors such as age, nutrition, and overall health significantly influence healing speed. Proper medical care during each phase ensures optimal recovery outcomes.
Possible Complications in Sever Wound Surgery Recovery
Although sever wound surgery is highly effective, complications may still occur during recovery. Infections are one of the most common risks, especially in deep or contaminated wounds. Poor healing may lead to delayed recovery or reopening of the wound. Nerve damage can result in loss of sensation or limited mobility in the affected area. Excessive scar tissue formation may restrict movement or cause cosmetic concerns. Blood clots may develop in severe trauma cases, requiring immediate medical attention. Graft rejection is another possible complication when skin grafts are used.
Rehabilitation and Functional Recovery
Rehabilitation plays a major role in restoring normal function after sever wound surgery. Physical therapy helps patients regain strength, flexibility, and mobility in affected areas. Occupational therapy supports the return to daily activities such as walking, dressing, or working. Exercises are often customized based on injury severity and surgical outcomes. Scar management techniques may be used to improve skin appearance and elasticity. Emotional and psychological support can also be important for patients recovering from traumatic injuries. Long-term rehabilitation ensures that patients regain independence and quality of life.
Special Patient Considerations
Certain patients require special attention during sever wound surgery and recovery. Individuals with diabetes often experience slower healing due to poor circulation and require strict monitoring. Elderly patients may have fragile skin and reduced regenerative ability, making recovery more complex. Children need carefully planned surgical approaches that consider growth and development. Patients with vascular diseases may face challenges due to reduced blood flow to injured areas. Each of these groups requires personalized treatment strategies to ensure safe and effective healing outcomes.
Modern Advances in Sever Wound Surgery
Modern medical technology has significantly improved outcomes in sever wound surgery. Negative pressure wound therapy helps accelerate healing by improving blood flow and removing excess fluid. Bioengineered skin substitutes provide new options for patients with extensive skin loss. Advanced imaging techniques allow surgeons to plan procedures with greater precision. Minimally invasive tools reduce surgical trauma and improve recovery times. Microsurgical techniques enable precise repair of small blood vessels and nerves. These innovations continue to improve survival rates and functional recovery in severe injury cases.
When Immediate Medical Attention Is Required
Immediate medical attention is necessary when a wound exposes deep tissues such as muscle or bone. Uncontrolled bleeding that does not stop with pressure requires urgent surgical evaluation. Signs of infection such as fever, redness, or pus formation indicate the need for immediate care. Loss of movement or sensation in a limb after injury suggests possible nerve or structural damage. Severe pain combined with swelling and discoloration may indicate internal complications. Prompt medical response increases the chances of successful treatment and recovery.
Preventive Measures for Severe Wound Injuries
Preventing injuries that lead to sever wound surgery involves safety awareness and protective measures. Wearing protective gear in workplaces and high-risk environments significantly reduces injury risks. Following road safety rules helps prevent accidents involving severe trauma. Proper handling of tools and equipment minimizes accidental injuries. Managing chronic conditions like diabetes reduces the risk of complications from minor wounds. Early treatment of small injuries prevents them from developing into severe medical conditions requiring surgery.
Frequently Asked Questions (FAQ)
What is sever wound surgery used for?
Sever wound surgery is used to treat deep and complex injuries involving muscles, tendons, bones, or blood vessels that cannot heal naturally.
How long does recovery take after sever wound surgery?
Recovery time varies depending on injury severity, but it can range from several weeks to several months.
Is sever wound surgery painful?
The procedure itself is not painful due to anesthesia, but mild to moderate pain may occur during recovery.
What are the risks of sever wound surgery?
Risks include infection, delayed healing, scarring, nerve damage, and complications from grafts.
Can all severe wounds be treated with surgery?
Most severe wounds require surgical intervention, but treatment depends on injury type and patient condition.
Is physical therapy necessary after surgery?
Yes, physical therapy is often essential to restore movement, strength, and function.
Takeaway
Sever wound surgery plays a critical role in modern trauma care by addressing complex injuries that cannot heal through basic treatment methods. Its success depends on timely intervention, precise surgical techniques, and careful post-operative care. Advances in medical technology continue to improve outcomes, making recovery more effective and less invasive for patients.