Understanding Decubitus Ulcers
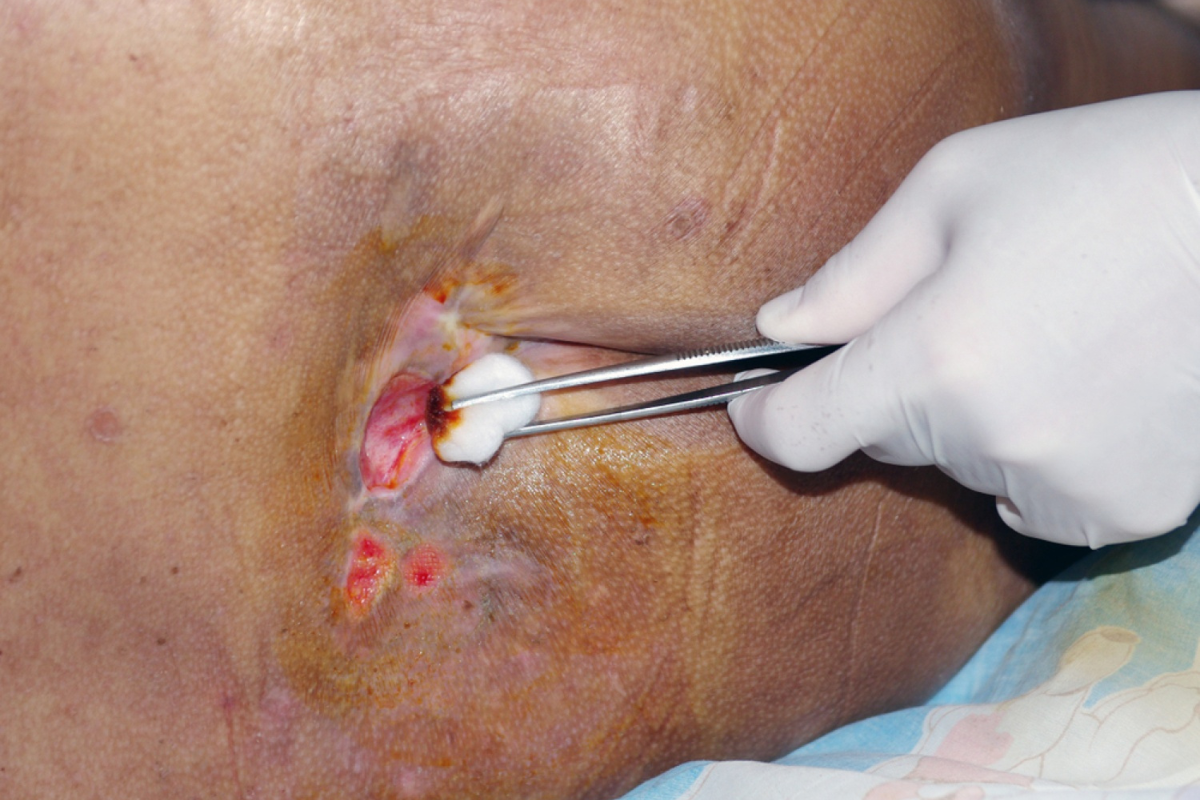
Decubitus ulcers, commonly known as pressure ulcers or bedsores, are injuries to the skin and underlying tissue caused by prolonged pressure. These wounds often develop in areas where bones are close to the skin, such as the heels, hips, tailbone, and elbows. When pressure restricts blood flow, the affected tissue becomes deprived of oxygen and nutrients, leading to damage over time. Individuals who remain in one position for extended periods are at the highest risk, especially those confined to beds or wheelchairs. Decubitus ulcer treatment begins with recognizing early signs like redness, tenderness, or skin discoloration. Without timely care, these wounds can progress into deeper and more severe injuries. Understanding how these ulcers form allows caregivers and patients to take proactive steps toward healing and prevention.
Causes and Risk Factors Behind Decubitus Ulcers
Several factors contribute to the development of pressure ulcers, making awareness essential for effective prevention and treatment. Prolonged immobility remains the primary cause, as it reduces circulation to vulnerable areas of the body. Friction and shear forces can also damage the skin when a patient slides or is repositioned improperly. Moisture from sweat or incontinence weakens the skin, increasing the likelihood of breakdown. Poor nutrition and dehydration further compromise the body’s ability to repair itself, slowing down the healing process. Medical conditions such as diabetes and vascular disease can also heighten the risk due to impaired blood flow. Elderly individuals and those with limited mobility are particularly vulnerable to these factors. Addressing these risks is a critical part of any decubitus ulcer treatment plan.
Stages of Pressure Ulcers and Their Characteristics
Pressure ulcers are categorized into stages based on their severity, which helps guide proper treatment strategies. Stage 1 ulcers appear as red or discolored areas that do not fade when pressed, signaling early tissue damage. In Stage 2, the skin may blister or break open, forming a shallow wound that requires immediate attention. Stage 3 ulcers extend deeper into the tissue, exposing fat and increasing the risk of infection. Stage 4 represents the most severe form, where damage reaches muscles, tendons, or even bone. Some wounds are classified as unstageable when covered by dead tissue, making it difficult to assess their depth. Deep tissue injuries may also develop beneath intact skin, appearing as dark or purplish areas. Identifying the stage accurately ensures that the chosen decubitus ulcer treatment is appropriate and effective.
Core Principles of Decubitus Ulcer Treatment
Successful decubitus ulcer treatment relies on a combination of medical care and supportive practices. The first priority is relieving pressure on the affected area to prevent further damage. Repositioning the patient regularly helps restore blood flow and supports healing. Protecting the wound from contamination is equally important to reduce infection risks. Maintaining a clean and properly dressed wound environment encourages tissue regeneration. Pain management also plays a role, as discomfort can limit mobility and slow recovery. Supporting overall health through proper nutrition and hydration enhances the body’s natural healing abilities. These principles form the foundation for managing both mild and severe pressure ulcers.
Wound Care Techniques for Decubitus Ulcer Treatment
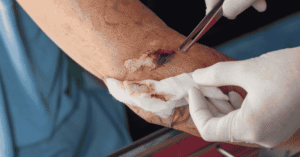
Proper wound care is essential for promoting healing and preventing complications. Cleaning the wound regularly helps remove debris and bacteria that can hinder recovery. Debridement is often necessary to eliminate dead tissue and stimulate new growth. Different methods, including surgical, enzymatic, and autolytic debridement, may be used depending on the severity of the ulcer. Choosing the right dressing is equally important, as it protects the wound and maintains an optimal healing environment. Moisture balance must be carefully managed to prevent dryness or excessive wetness. Frequent monitoring allows caregivers to adjust treatment as needed. Consistent wound care is one of the most effective ways to support successful decubitus ulcer treatment.
Common Wound Care Practices
- Cleaning the wound with saline or prescribed solutions
- Applying appropriate dressings based on wound stage
- Removing dead tissue through safe debridement methods
- Monitoring for signs of infection such as redness or odor
- Keeping the surrounding skin clean and dry
- Changing dressings as recommended by healthcare providers
- Documenting progress to track healing improvements
Advanced Medical Treatments for Pressure Ulcers
In more severe cases, advanced medical interventions may be required to support healing. Negative pressure wound therapy is a widely used technique that promotes tissue growth by applying controlled suction. Biologic dressings and growth factors can help accelerate the repair process by stimulating cell regeneration. Hyperbaric oxygen therapy delivers high levels of oxygen to the wound, enhancing healing in certain cases. Surgical options such as skin grafts or flap procedures may be necessary for deep or non-healing ulcers. These treatments are typically recommended when standard care methods are not sufficient. Close monitoring by healthcare professionals ensures that complications are managed effectively. Access to advanced therapies can significantly improve outcomes in complex decubitus ulcer treatment scenarios.
Pain Management and Patient Comfort
Managing pain is a vital component of treating pressure ulcers, as discomfort can interfere with recovery. Patients may experience varying levels of pain depending on the severity of the wound. Medications such as analgesics or anti-inflammatory drugs are often prescribed to provide relief. Non-pharmacological approaches, including repositioning and supportive cushions, can also reduce discomfort. Gentle handling during wound care procedures minimizes additional pain and stress. Emotional support is equally important, as chronic wounds can affect mental well-being. Creating a comfortable environment encourages cooperation and improves overall quality of life. Addressing pain effectively enhances the success of decubitus ulcer treatment.
Role of Nutrition in Healing Pressure Ulcers
Nutrition plays a crucial role in the body’s ability to repair damaged tissue. Protein is essential for rebuilding skin and supporting immune function. Vitamins such as Vitamin C aid in collagen production, while zinc helps with wound healing. Iron supports oxygen transport, which is necessary for tissue regeneration. Staying hydrated keeps the skin healthy and resilient. Patients with poor appetite or dietary restrictions may require nutritional supplements to meet their needs. A balanced diet tailored to the individual’s condition can significantly speed up recovery. Integrating proper nutrition into decubitus ulcer treatment ensures a more comprehensive approach to healing.
Preventive Strategies to Avoid Recurrence
Preventing pressure ulcers from recurring is just as important as treating existing wounds. Regular repositioning reduces prolonged pressure on vulnerable areas of the body. Specialized mattresses and cushions provide additional support and help distribute weight evenly. Daily skin inspections allow for early detection of potential problems. Maintaining proper hygiene keeps the skin clean and less prone to breakdown. Managing moisture levels is essential, especially for patients with incontinence. Educating caregivers and patients about preventive measures fosters consistency in care. These strategies are key to long-term success in decubitus ulcer treatment.
Home Care vs Professional Medical Treatment
Deciding between home care and professional treatment depends on the severity of the ulcer. Early-stage wounds can often be managed at home with proper guidance and attention. Caregivers play a critical role in maintaining hygiene, repositioning, and monitoring progress. However, advanced ulcers require medical expertise to prevent complications. Signs such as increased pain, foul odor, or signs of infection should prompt immediate medical attention. Regular follow-ups ensure that the treatment plan remains effective. Collaboration between caregivers and healthcare professionals provides the best outcomes. Choosing the right level of care is essential for safe and effective decubitus ulcer treatment.
Common Challenges in Decubitus Ulcer Treatment
Treating pressure ulcers can present several challenges that require patience and consistency. Chronic conditions such as diabetes can slow the healing process and increase complications. Infections remain a significant concern, especially in advanced stages of ulcers. Limited mobility can make repositioning difficult, affecting recovery progress. Patient compliance is another factor, as consistent care is necessary for improvement. Financial constraints may also impact access to advanced treatments or specialized equipment. Emotional stress for both patients and caregivers can add to the difficulty of managing long-term wounds. Overcoming these challenges requires a comprehensive and adaptable approach to decubitus ulcer treatment.
Frequently Asked Questions
What is the fastest way to heal a decubitus ulcer
The fastest approach involves relieving pressure, maintaining proper wound care, and ensuring adequate nutrition. Combining these methods supports faster tissue repair and reduces complications.
Can decubitus ulcers be treated at home
Early-stage ulcers can often be managed at home with proper care, but more severe cases require professional medical attention to avoid serious complications.
How long does decubitus ulcer treatment take
Healing time varies depending on the severity of the ulcer and the patient’s overall health. Some wounds may heal in weeks, while others can take months.
What are the warning signs of infection in a pressure ulcer
Common signs include redness, swelling, warmth, foul odor, pus, and fever. Immediate medical attention is necessary if these symptoms appear.
Are pressure ulcers preventable
Yes, consistent repositioning, proper skin care, and the use of supportive surfaces can significantly reduce the risk of developing pressure ulcers.
What type of mattress is best for preventing pressure ulcers
Alternating pressure mattresses and high-density foam mattresses are commonly recommended for reducing pressure and improving comfort.
Takeaway
Decubitus ulcer treatment requires a well-rounded approach that combines proper wound care, pressure relief, nutrition, and medical support. Early detection and consistent care significantly improve healing outcomes and reduce the risk of complications. Caregivers and patients must work together to maintain hygiene, monitor progress, and follow recommended treatment plans. Advanced therapies offer additional options for severe cases, providing hope for improved recovery. Prevention remains a key focus, as avoiding recurring ulcers enhances long-term health and comfort. With the right knowledge and dedication, managing pressure ulcers becomes more effective and less overwhelming.